Strengthening hand hygiene in Uganda’s healthcare facilities
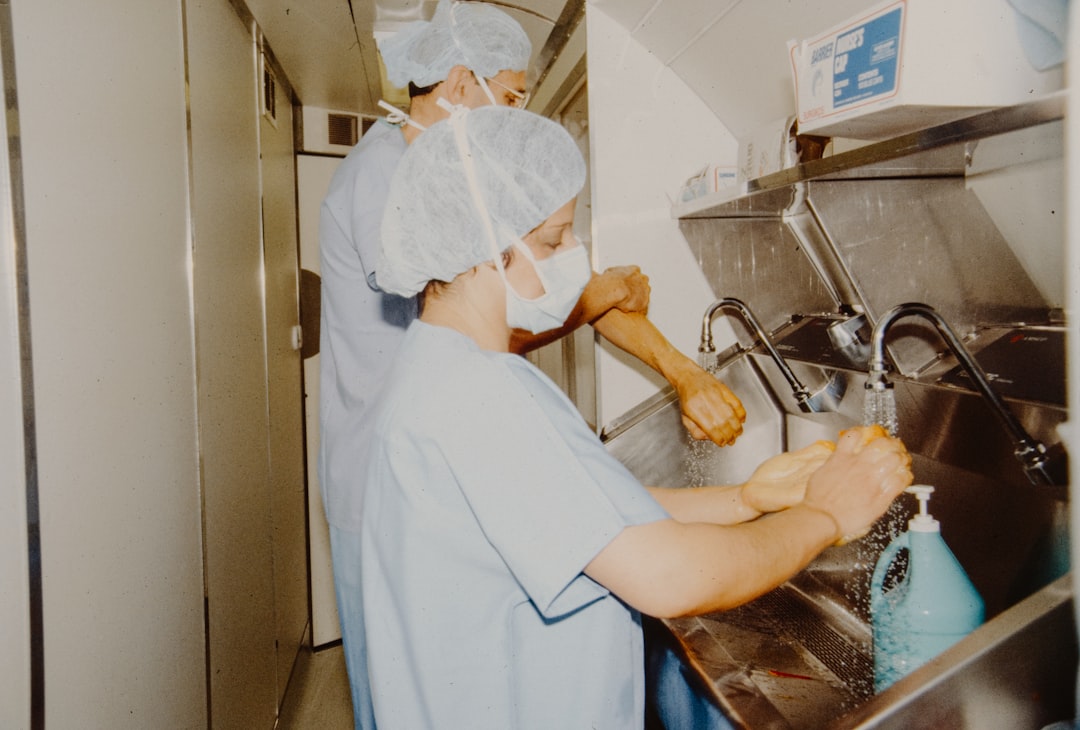
Efforts in Uganda improve hand hygiene in healthcare with Alcohol-Based Hand Rub (ABHR) production, addressing gaps in infection control.
The importance of hand hygiene has been made abundantly clear, particularly in healthcare environments where the stakes are highest. In Uganda, the focus on hand hygiene has found tangible expression through a project aimed at addressing the gaps in healthcare infection control—primarily through the localized production and access to Alcohol-Based Hand Rub (ABHR). This effort, spearheaded by the Infectious Disease Institute (IDI) at Makerere University, underscores the role of behavioral interventions, resource accessibility, and healthcare worker engagement in preventing infections.
The Problem: Healthcare-Associated Infections
Worldwide, healthcare-associated infections (HAIs) are a significant burden. According to the World Health Organization (WHO), at least 10 out of every 100 patients in healthcare settings in low- and middle-income countries acquire infections during their stay. Intensive Care Units (ICUs), in particular, report higher rates, with 30% of all infections linked to these settings. Hand hygiene plays a pivotal role in preventing such infections, making it a cornerstone in infection prevention and control (IPC).
However, compliance with hand hygiene protocols remains a persistent challenge. Healthcare workers often fail to adhere to recommended practices despite knowing their importance. The reasons are multifaceted, including a lack of accessibility to hand hygiene products, insufficient training, fatigue, and the sheer demands of busy healthcare settings.
An Innovative Approach: Alcohol-Based Hand Rub Production
Recognizing these issues, Uganda turned to a localized solution: the production of Alcohol-Based Hand Rub (ABHR) as a cost-effective and efficient measure to bridge gaps in infection control.
The Steps to Implementation
Sheila Natto, Senior Technical Advisor for Infection Prevention and Control at IDI, highlighted the structured approach taken to implement the ABHR initiative:
- Leadership Buy-In: Engaging hospital leadership was the first step. Leadership teams were brought on board to understand the critical importance of hand hygiene and its correlation to preventing infections.
- Baseline Assessments: Infection Prevention and Control (IPC) committees conducted baseline assessments in healthcare facilities. These assessments identified gaps in hand hygiene practices and resources.
- Training and Planning: Healthcare workers, including IPC committee members, underwent targeted training programs. Facility work plans were developed to incorporate regular hand hygiene monitoring, ABHR usage audits, and follow-up assessments.
- Monitoring and Feedback Loops: Facilities integrated hand hygiene monitoring into IPC programs, including observing compliance to WHO guidelines—before and after patient contact.
Key Milestones of the ABHR Initiative
- Local Production: The production of ABHR followed WHO guidelines to meet safety and efficacy standards. Facilities were equipped with the infrastructure to produce ABHR locally, ensuring a steady supply while reducing dependency on external sources.
- Targeted Training: Training sessions helped healthcare workers understand not only the proper usage of ABHR but also its role in reducing patient infections. This emphasis on behavior change was critical to the initiative's success.
- Strategic Placement: ABHR dispensers were installed at key points of care—hospital wards, entry points, and high-risk areas like ICUs—where quick access could aid compliance. Healthcare workers were also provided with pocket-sized ABHR bottles for convenience.
- Extended Distribution: Beyond hospitals, the initiative included distribution to community healthcare settings and high-risk locations, further extending its impact.
Outcomes: Compliance and Convenience
Careful monitoring and assessments have shown gradual improvements in hand hygiene compliance. Using WHO’s observation tools, data collected before and after implementing the ABHR initiative revealed that:
- Compliance rates in healthcare settings increased over time at both mid-point and endpoint evaluations.
- The integration of ABHR addressed critical limitations like limited availability of soap and water in high-demand settings.
- Workers appreciated the convenience of ABHR as it saved time, particularly in busy environments.
Addressing Behavioral and Logistical Barriers
Behavior change and logistical challenges were key considerations. Healthcare workers reported that having ABHR dispensers readily accessible on trolleys and in wards reduced the time needed to take trips to washing basins. Additionally, pocket-sized ABHR bottles acted as a constant reminder, reinforcing the habit of hand hygiene even during hectic shifts.
Another significant advantage of locally-produced ABHR was that it bypassed supply chain disruptions. District-level production ensured consistent availability, reducing reliance on imports and accelerating delivery times to facilities in need.
The Role of Partnerships
None of this would have been possible without collaboration among Uganda’s Ministry of Health, district-level leadership, and international partners such as the U.S. Centers for Disease Control and Prevention (CDC). Each stakeholder contributed to different facets of the program: from policy support and capacity building to funding and logistical aid.
Expanding the Reach
The initiative also drew attention to the need for hand hygiene access in community settings. Community healthcare workers, who operate at the grassroots level, received ABHR supplies to promote hand hygiene at the local level. This approach extends the benefits of stronger hand hygiene practices beyond hospitals, targeting broader public health improvements.
Challenges and Lessons Learned
While the initiative has demonstrated significant strides in improving hand hygiene compliance, challenges remain. Sustainable financing, maintaining consistent quality during local production, and expanding community outreach represent ongoing hurdles. Scaling production to meet the needs of larger hospitals and rural clinics alike remains a work in progress.
Additionally, existing cultural and behavioral barriers emphasize the need for ongoing health education, not only among healthcare workers but also patients and caregivers, to embed the practice of hand hygiene into daily care routines.
Why It Matters
The Ugandan initiative demonstrates how targeted, localized action can profoundly impact the quality of healthcare delivery. By focusing on sustainable and practical solutions like ABHR production and distribution, the program addresses systemic issues while fostering behavioral change.
Healthcare-associated infections cost human lives and economic resources. Simple measures like improving hand hygiene, when supported by robust infrastructure and policy leadership, can save lives and minimize financial strain on both patients and healthcare systems. For other nations grappling with similar issues, Uganda’s approach provides a blueprint of how healthcare priorities can be advanced through thoughtful planning, multi-stakeholder collaboration, and a relentless focus on behavioral and systemic improvements.
Staff Writer
Ryan reports on fitness technology, nutrition science, and mental health.
Comments
Loading comments…



